Overview
Colposcopy is an exam or test done for the well-being of the female reproductive tract. In this test your cervix, vagina, and vulva for any abnormality or signs of disease. A colposcope is a special instrument used to perform this procedure by your doctor.
This fairly simple procedure is usually done as a screening procedure to find any abnormal cells in your cervix, which can be a sign of cervical cancer. This test helps you get prompt treatment. In this article, we will discuss colposcopy and its procedure.
Indications
Your doctor may prescribe you a colposcopy in a few situations:
- Abnormal vaginal bleeding
- Pain around your vulva or in your perineum (the body area between your thighs)
- Genital warts – this test can be used to diagnose your genital warts which can be due to certain causes
- If you have an abnormal Pap test or pelvic exam – a pap test or pap smear test is used to assess the health of your cervix. It is done to check the cells of the junction between your uterus and cervix. If the pap smear showed abnormal types of cells.
- Suspicion of cervical cancer
- Suspicion of vulvar cancer
- Abnormal discharge from your vagina
Risks of Procedure
Colposcopy is usually a risk-free procedure. If your doctor has prescribed you to have biopsies (taking or excising tissue sample for further tests) during this test, some rare complications that may arise are:
- Heavy or abnormal bleeding – this can happen from the site where the biopsy was taken from
- Infection – infections can rarely arise especially if you have a weakened immune system. These infections show up as fever (high), severe pain, and/or bleeding.
- Pelvic pain – pelvic pain can be caused by an injury to your reproductive system or an infection.
In case you experience the following symptoms make sure to call your doctor immediately:
- High fever and chills
- Bleeding that is more than your usual menstrual bleeding
- Severe pelvic or abdominal pain
Patient Preparation
Most of the preparations required for colposcopy are easy to follow. Apart from physical preparation, some people may require mental preparation for this test as you may feel anxiety before getting a colposcopy. Your doctor may recommend you the following:
- Avoid scheduling your examination during your periods
- Change into a hospital gown or undress waist down
- Should avoid sexual intercourse a day or two before your colposcopy
- Avoid the use of tampons two days before your colposcopy
- Don’t use any topical vaginal medication/creams for two days before your test
- Take an over-the-counter pain killer e.g., ibuprofen or acetaminophen when you’re coming to get your colposcopy
Many women are sensitive about getting any vaginal or pelvic examinations. They can anxiety the day of or a couple of days before their exam. To alleviate this anxiety you should:
- Discuss the test thoroughly with your doctor and ask them about what you should expect. You can also ask them for any brochures or pamphlets with all the details about colposcopy.
- Ask your doctor about any concerns or questions that you have about the test e.g., is it painful or uncomfortable?
- You can do activities that make you relax e.g., exercise, yoga, or talking to your best friend
Procedure
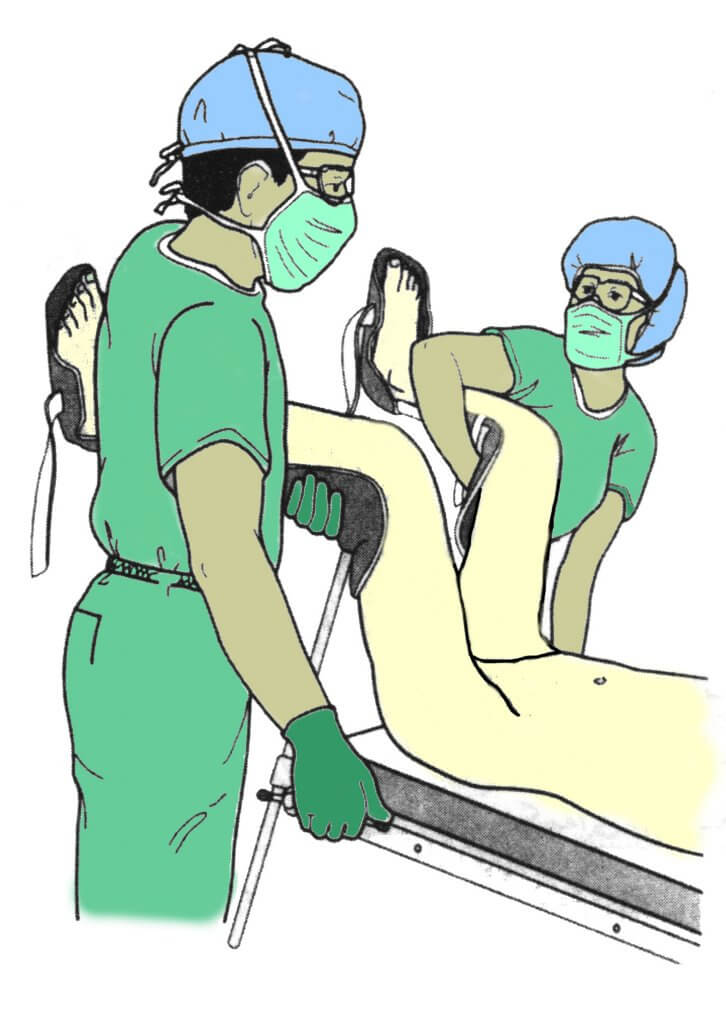
Colposcopy is usually done in a doctor’s office or clinic. This procedure usually takes about 10 to 20 minutes. Similar to the pap smear (pelvic exam), during the procedure you’ll lie on the table with your back flat and your legs raised and supported (by stirrups) also called a lithotomy position.
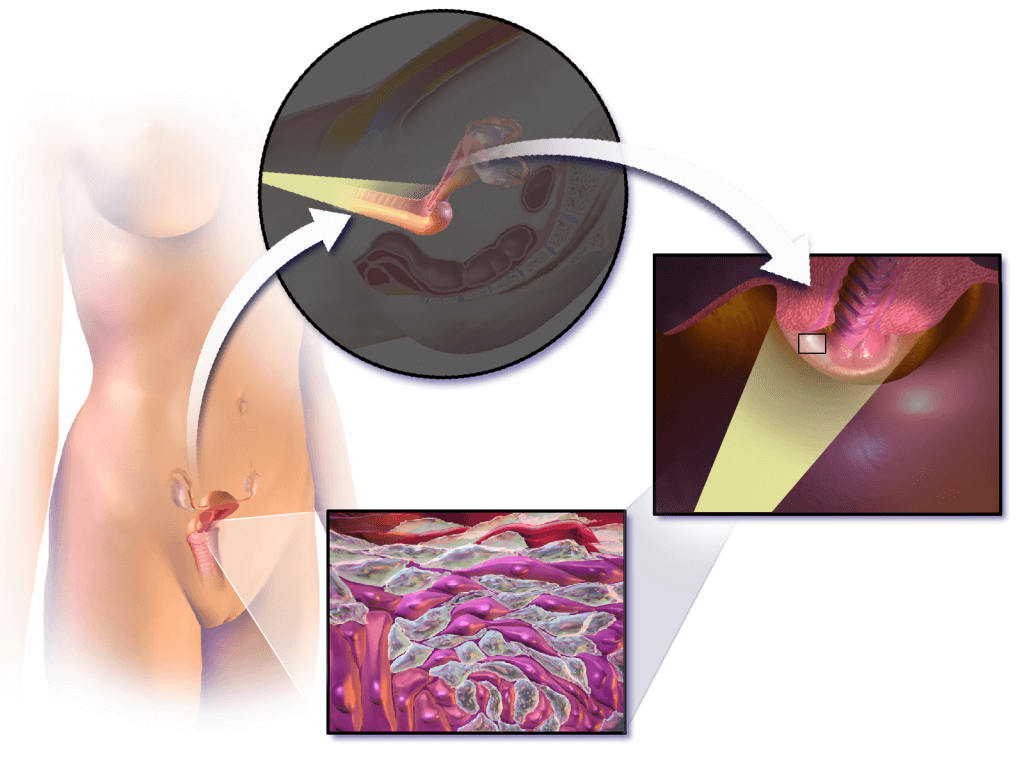
After confirming that you’re comfortable, your doctor will then place a metal speculum in your vagina. This (Cusco’s) speculum is a bivalve, i.e., it has metal strips that hold your vaginal walls apart during the procedure and makes your vagina and cervix visible to the doctor. Insertion of the speculum can make you feel a little bit uncomfortable and may cause you slight pain. You can ask your doctor to stop if you are having a lot of pain during this procedure.
Your doctor will now place the colposcope a few inches away from your vulva. The colposcope is a special magnifying instrument (as binoculars) that shines light and lets your doctor look at your cervix.
The doctor will then clean any excess mucus from your cervix. Your doctor may apply a certain solution to the areas being examined, highlighting the suspicious cells. You may feel a burning or tingling sensation.
In case there is a suspicious or abnormal tissue your doctor may take a biopsy. Your doctor will use a sharp biopsy tool (scalpel). If there are multiple abnormal tissue sites, your doctor may take multiple biopsies. Biopsies can be a little uncomfortable:
- Cervical biopsy – a biopsy taken from your cervix or upper part of the vagina will cause you mild to moderate discomfort, however, it is usually pain-free. Usually, some pressure or cramping may be felt.
- Vaginal biopsy – a biopsy from the lower part of your vagina or vulva can cause pain and your doctor will most likely use a local anaesthetic or numbing cream on that area.
Patient Recovery
Colposcopy procedures without biopsies are simple and you can go home without any special restriction. You may experience spotting or very light bleeding from your vagina.
In case your doctor took biopsies, you may:
- Experience some vaginal or vulvar pain for a day or two
- Have light bleeding from your vagina lasting a few days
- See a dark coloured discharge from your vagina
- You should avoid wearing tampons, douching, and having sexual intercourse for as long as your doctor tells you (usually a week).
Outcomes
If your doctor did not see any abnormalities they will let you know right after your test.
If your doctor took any samples or biopsies, the results might take up to two weeks or so to come. You should ask your doctor about what to expect from the results. Your results can show certain conditions:
- Human papillomavirus (HPV) infection
- STDs like gonorrhoea, chlamydia
- Pelvic inflammatory disease (PID)
- Cervical cancer or precancerous state of the cervix
- Vulvar or vagina cancer
According to your results, your doctor will prescribe you further testing or evaluation.
- Frequently asked questions: Special procedures FAQ 135: Colposcopy. The American College of Obstetricians and Gynecologists. https://www.acog.org/Patients/FAQs/Colposcopy?IsMobileSet=false. Accessed Oct. 1, 2019.
- Feltmate CM, et al. Colposcopy. https://www.uptodate.com/contents/search. Accessed Oct. 1, 2019.
- Lobo RA, et al. Intraepithelial neoplasia of the lower genital tract (cervix, vagina, vulva): Etiology, screening, diagnosis, management. In: Comprehensive Gynecology. 7th ed. Elsevier; 2017. https://www.clinicalkey.com. Accessed Oct. 1, 2019.
- Smith RP. Colposcopy. In: Netter’s Obstetrics and Gynecology. 3rd ed. Elsevier; 2018. https://www.clinicalkey.com. Accessed Nov. 12, 2019.
- Fowler GC, et al., eds. Colposcopic examination. In: Pfenninger and Fowlers’ Procedures for Primary Care. 4th ed. Elsevier; 2020. https://www.clinicalkey.com. Accessed Oct. 1, 2019.
- Abdelhakim AM, et al. Effect of music in reducing patient anxiety during colposcopy: A systematic review and meta-analysis of randomized controlled trials. Journal of Gynecology Obstetrics and Human Reproduction. 2019; doi:10.1016/j.jogoh.2019.07.007.
- Khan MJ, et al. ASCCP colposcopy standards: Role of colposcopy, benefits, potential harms, and terminology for colposcopic practice. Journal of Lower Genital Tract Disease. 2017; doi:10.1097/LGT.0000000000000338.
The content shared in the Health Literacy Hub website is provided for informational purposes only and it is not intended to replace advice, diagnosis, or treatment offered by qualified medical professionals in your State or Country. Readers are encouraged to confirm the information provided with other sources, and to seek the advice of a qualified medical practitioner with any question they may have regarding their health. The Health Literacy Hub is not liable for any direct or indirect consequence arising from the application of the material provided.