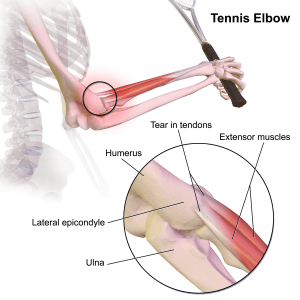
Overview
Varicose veins occur when veins in any part of the body become over-dilated and engorged with blood. They are small and visible through the skin’s surface and have a dark red or blue hue. Varicose veins are mostly known for their twisted appearance. A milder form of varicose veins are spider veins for their smaller web-like appearance and most commonly appear on the face and legs. Varicose veins are found in parts of the body that sustain a lot of pressure in their vessels such as the legs. Varicose veins usually do not pose a health threat and are mostly treated for cosmetic reasons.
Varicose veins occur up to 73% in women and up to 56% in women. In Australia, 10.4-23.0 % of men and 29.5-39.0% of women have a form of varicose veins. In this article, we will dive into what causes varicose veins and the treatment options available.
Signs and Symptoms
Varicose veins usually do not cause any pain or discomfort. This, however, may not always be the case. In the situation, that these veins do cause pain some signs to look out for are:
- Red, blue, and dark blue veins – due to deoxygenated blood inside
- Bulging cord-like tangled veins – due to pooling of blood
- A heavy aching feeling in legs
- A burning, cramping, pulsating feeling in legs
- Itchiness surrounding veins
- Skin discoloration surrounding veins
Causes
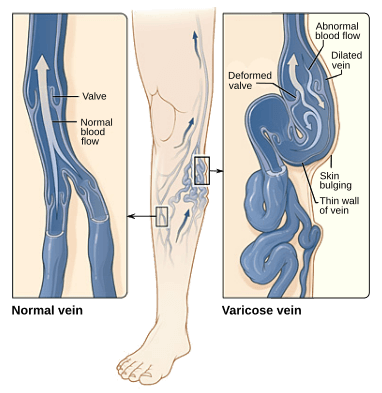
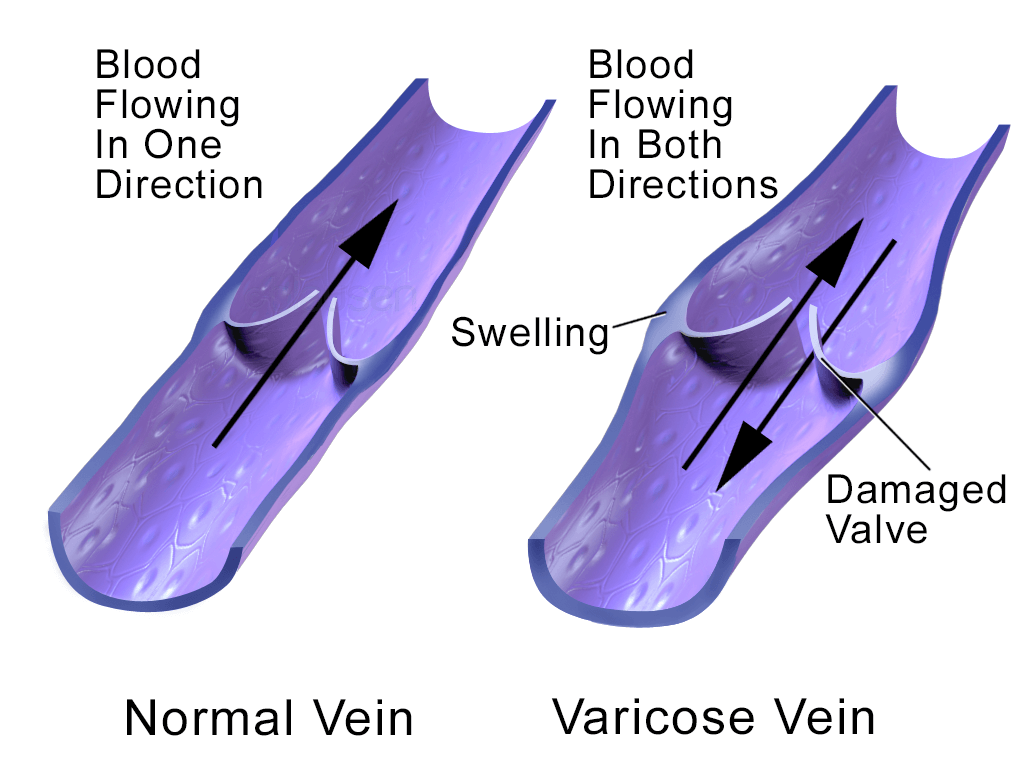
Arteries are used for carrying blood to the tissue of the body. This blood once it transfers oxygen and vital nutrient must return to the heart. To return to the heart, veins are used to carry blood against gravity back to the heart. There is two way in which flow against gravity is enhanced. Muscle contractions in the lower leg help push blood back up the leg through the veins. Secondly, valves within the vein maintain ‘one-way’ blood flow up back to the heart.
As stated before, varicose veins are caused by an increase of pressure within the blood vessel. This increased blood pressure causes the valves within the vein to become weakened. These valves are primarily utilized for the movement of blood in one direction. However, if these valves become weakened, the blood then moves backward. With this backward movement, the blood becomes pooled within the vessel. This then causes the formation of enlarged vessels on the skin surface (superficial surface). These vessels then give a distinctive dark purple or blue color which is visible to the human eye.
Risk Factors
Some risk factors are associated with an increased likelihood of developing varicose veins. The factors include:
- Age – as a person ages, the individual’s blood vessels weaken. This is due to prolonged life-long wearing out of valves in veins. With enough damage, the valves stop doing their job and let blood backflow causing blood vessels to become enlarged.
- Sex – women have a higher tendency of developing varicose veins. This is due to the fact that female hormones such as estrogen and progesterone both relax and slacken vein walls. This causes blood to more easily pool within the vein. Hormonal changes due to oral contraceptives and pregnancy may increase the likelihood of developing varicose veins.
- Pregnancy – in pregnancy, the total blood volume of a woman becomes nearly one and half times the amount while not pregnant. This sudden increase in total volume causes strain on the veins. The stretching of blood vessels can consequently cause the enlargement of veins.
- Genetic – if any family members more easily form varicose veins then the likelihood of you forming varicose veins increase as well.
- Obesity – elevated body weight increases the pressure that is applied onto your veins.
- Being immobile for a long amount of time – if you are sitting or standing too long, the blood flow in your legs is not as good as if you were to move around.

Complications
Complications from varicose veins are a rare occurrence but can still occur. The complications are as follows:
- Ulcers – a sore can form on the skin surface near varicose veins. These sores can then develop into ulcers and mostly occur near the ankle.
- Blood clots – if blood engorges a blood vessel too long, this may cause a blood clot to start forming which is life-threatening.
- Bleeding – because varicose veins are so close to the skin surface, a burst in the vessel may cause bleeding though mostly minor.
Diagnosis
To diagnose whether or not you have varicose veins, your physician will do a physical exam and ask questions about the pains you experience. To make sure there is not too much damage to your valves, your doctor may do an ultrasound. In an ultrasound, a smooth handheld device is glided over the area suspected to have varicose veins to properly form an image of the veins in your leg.
Treatment
A lot of symptoms of varicose veins can be reversed by proper self-care and compression stockings but if they become out of hand, there are some options available such as:
- Sclerotherapy – a solution or foam is injected into a medium-sized vein to cause it to close up and over the next few weeks, the veins fade.
- Laser therapy – This therapy is used to get rid of smaller varicose veins or spider veins
- Cather-assisted therapies using radiofrequency – A catheter is inserted into a large vein. The radiofrequency then shuts off the blood flow in the vein.
- High ligation – A vein is sealed off and eventually stopped from joining a deep vein via incisions.
- Phlebectomy – Small veins are punctured and destroyed under local anesthesia.
- Endoscopic vein surgery – This treatment is used when all other fail and an ulcer has formed. A camera is inserted into your leg and the vein is then removed by small incisions.
Prevention
There is no clear way to prevent these veins from forming but here are some steps you can take to decrease the chance of them forming, including:
- Exercising regularly
- Changing positions often
- Raising legs while sitting or laying
- Avoiding tight clothing and high-heels
- Maintaining good body weight
- Avoiding high-salt food to decrease high blood pressure which may cause swelling in blood vessels
When to see a doctor
In most cases, prevention and self-care can help you correct the varicosity of your veins. These measures include. However, if you are still concerned about the appearance of varicose veins, you can go to your doctor and consult for the different treatment options.
- Papadakis MA, et al., eds. Blood vessel & lymphatic disorders. In: Current Medical Diagnosis & Treatment 2021. 60th ed. McGraw Hill; 2021. https://accessmedicine.mhmedical.com. Accessed Dec. 11, 2020.
- Varicose veins. National Heart, Lung, and Blood Institute. https://www.nhlbi.nih.gov/health-topics/varicose-veins. Accessed Dec. 11, 2020.
- AskMayoExpert. Varicose veins. Mayo Clinic; 2018.
- Varicose veins and spider veins. National Women’s Health Information Center. https://www.womenshealth.gov/a-z-topics/varicose-veins-and-spider-veins. Accessed Dec. 10, 2018.
- Kabnick LS, et al. Overview of lower extremity chronic venous disease. https://www.uptodate.com/contents/search. Accessed Dec. 11, 2020.
- Kang S, et al., eds. Treatment for varicose and telangiectatic lower extremity vessels. In: Fitzpatrick’s Dermatology. 9th ed. McGraw Hill; 2019. https://accessmedicine.mhmedical.com. Accessed Dec. 11, 2020.
- Grape. Natural Medicines. https://naturalmedicines.therapeuticresearch.com. Accessed Dec. 11, 2020.
- Sweet clover. Natural Medicines. https://naturalmedicines.therapeuticresearch.com. Accessed Dec. 11, 2020.
- Horse chestnut. Natural Medicines https://naturalmedicines.therapeuticresearch.com. Accessed Dec. 11, 2020.
- Butcher’s broom. Natural Medicines. https://naturalmedicines.therapeuticresearch.com.Accessed Dec. 11, 2020.
- Alguire PC, et al. Medical management of lower extremity chronic venous disease. https://www.uptodate.com/contents/search. Accessed Dec. 11, 2020.
- Riggin EA. AllScripts EPSi. Mayo Clinic, Dec. 14, 2020.
- Jennifer L. Beebe-Dimmer, John R. Pfeifer, Jennifer S. Engle, David Schottenfeld, The Epidemiology of Chronic Venous Insufficiency and Varicose Veins, Annals of Epidemiology, Volume 15, Issue 3, 2005, Pages 175-184, ISSN 1047-2797.
- https://www.health.gov.au/resources/pregnancy-care-guidelines/part-i-common-conditions-during-pregnancy/varicose-veins
The content shared in the Health Literacy Hub website is provided for informational purposes only and it is not intended to replace advice, diagnosis, or treatment offered by qualified medical professionals in your State or Country. Readers are encouraged to confirm the information provided with other sources, and to seek the advice of a qualified medical practitioner with any question they may have regarding their health. The Health Literacy Hub is not liable for any direct or indirect consequence arising from the application of the material provided.