Overview
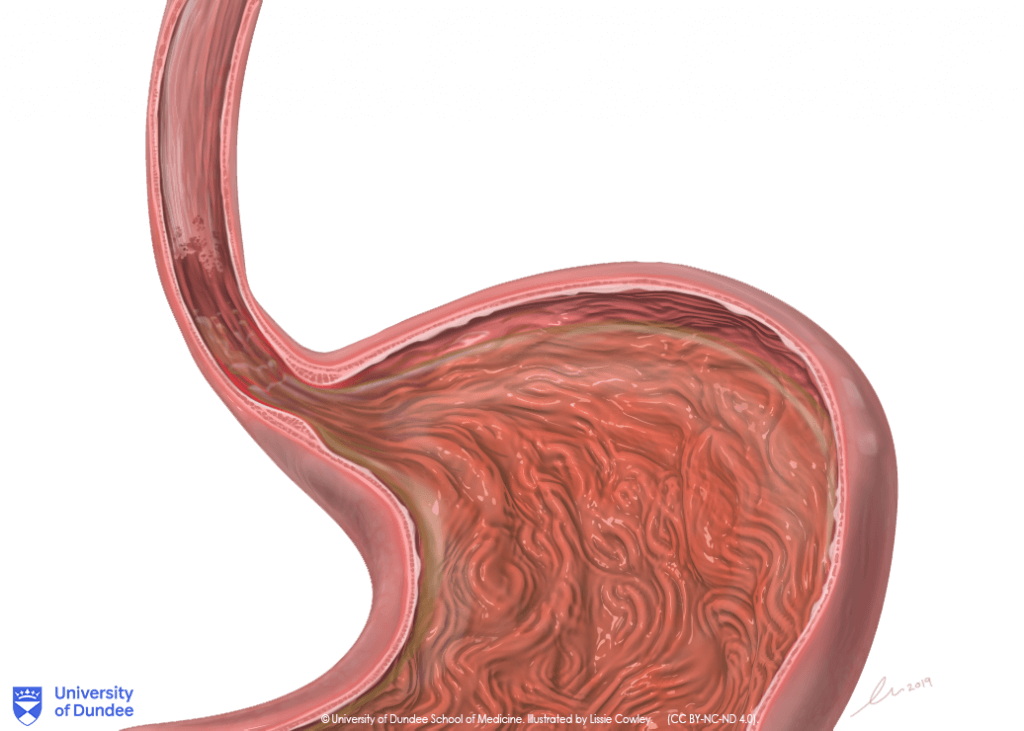
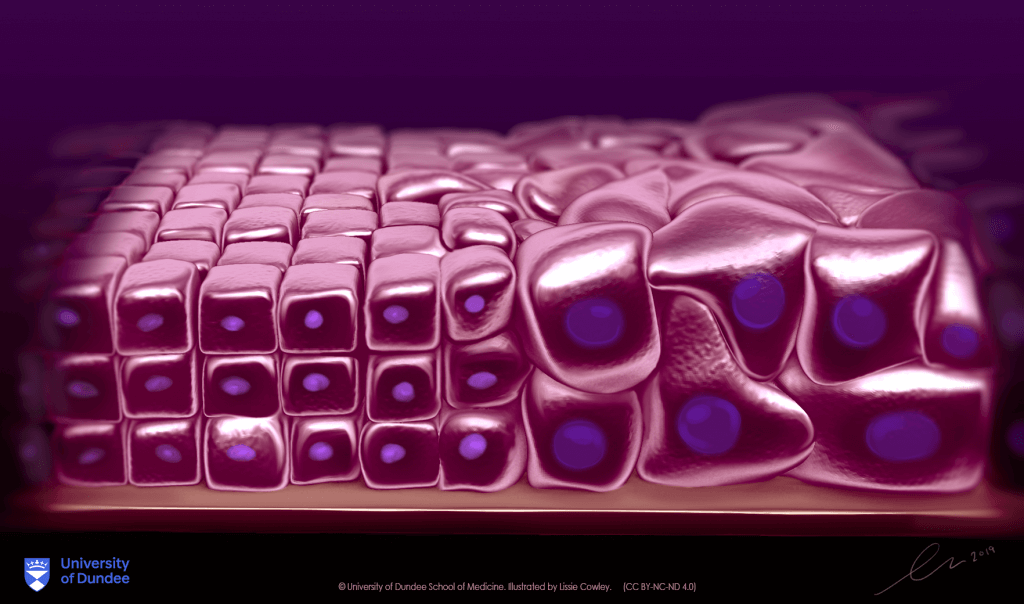
Dysplasia refers to an abnormal change in the morphology (appearance) of cells within a tissue or an organ. It can occur in any tissue of the body. Oesophageal dysplasia is also known as Barret’s Oesophagus and is the abnormal change in the cell lining your oesophagus i.e., your food tube that carries food from the throat to the stomach. The oesophagus is located in the mediastinum and is part of the digestive system.
For unknown reasons, the oesophageal cell lining develops into more of an intestinal-like lining.
Dysplasia should not be considered as cancer (metaplasia); however, it can predispose a person to cancer. Barret’s oesophagus is present in almost 1% of the people around the globe affecting male white people more than others. Moreover, middle-aged or older people experience this condition more than young people.
In this article, we will discuss what oesophageal dysplasia is and how you can diagnose it, treat it, and even prevent it in the first instance!
Signs and Symptoms
Oesophageal Dysplasia often goes symptomless. You only figure out that you have this pathology (disease) if you get checked for GERD (gastroesophageal reflux disease), or you have already developed cancer. However, you can watch for the signs associated with this disease. These include heartburn (long-term) and acid regurgitation (burning sensation while burping and vomiting in the back of your throat).
Symptoms are associated with other diseases but heartburn occurring twice a week or more is a big red flag. Other symptoms may include:
- Heartburn – worsening during sleep or wakes you up from sleep
- Dysphagia – difficulty or pain in swallowing food
- A sensation of food not passing down to your stomach
- Constant sour taste in your mouth or bad breath
- Vomiting
- Unintentional weight loss
Causes and Risk Factors
Various factors can contribute to Oesophageal dysplasia. One of the most common causes is GERD. Gastroesophageal reflux disease (GERD) is a chronic condition in which the acidic content of your stomach flows back into your oesophagus causing damage to it. Eating smoked food e.g., B.B.Q. or grilled food is also linked to oesophageal and stomach dysplasia that can lead to cancer. Some risk factors for GERD are:
- Smoking
- Obesity
- Eating large processed meals
- Drinking too much caffeine or tea
- Drinking alcohol
- Lying down right after taking a meal
- Pregnancy
These risk factors can eventually lead to Barret’s oesophagus. However, you can have this condition without having GERD.
Complications
Most people don’t have to worry about oesophageal dysplasia turning into cancer. However, 10% of people carry a high risk of developing cancer. Any cell behaving or growing abnormally has a high chance of turning into cancer, eventually leading to poor prognosis (outcome of the disease).
You can also experience heavy bleeding if your oesophagus gets ruptured leading you to a shock that can be fatal.
Diagnosis
Your doctor would ask you to go under a test called an upper endoscopy. Endoscopy is a procedure in which your internal organs are visualised using a camera inserted via a tube from your throat. The appearance of the lining of the oesophagus can hint at dysplasia, however, the only way to confirm the presence of oesophageal dysplasia is to take a small tissue sample (biopsies) and test them in the lab. These biopsies are seen under a microscope to confirm the changes in the cells.
A pathologist (specialist of diseases) will confirm if you have Barret’s Oesophagus.
Treatment
The treatment of oesophageal dysplasia depends largely on the degree of the severity of symptoms and dysplasia seen in biopsies. Dysplasia can be divided into:
- Low-grade dysplasia
Low-grade dysplasia refers to the presence of some abnormal cells. The majority of cells, however, are not affected. At this stage, your doctors will keep you under monitoring. The treatment at this stage is mostly lifestyle changes and medications that reduce the acid reflux from your stomach. You may be advised to:
- Eat whole food
- Avoid spicy, smoked, and processed food
- Eat small meals throughout the day
- Increase physical activity
- Drink more water and fewer beverages like alcohol, caffeine
- Reduce weight
- Medication – drugs like antacids that reduce the production of acid in the stomach.
You would also be required to get an endoscopy done every two to three years to monitor the extent of your oesophageal dysplasia.
- High-grade dysplasia
This form of dysplasia indicates a considerable change in your oesophageal lining. You are more likely to develop cancer if you have high-grade oesophageal dysplasia. You need to have more frequent upper endoscopies to screen for cancer. Your health provider may recommend different treatment regimens:
- Radiofrequency ablation – the most common procedure. It works by burning the abnormal tissue using radio waves, which generate heat.
- Cryotherapy – it is a procedure in which liquid nitrogen is introduced to the diseased parts in an attempt to freeze the diseased parts of the oesophageal lining so it will shed off
- Endoscopic mucosal resection – your doctor can remove the precancerous spots on the oesophageal lining using an endoscope
- Surgery – complete resection may be required if you have a severe grade of oesophageal dysplasia. The procedure is called esophagectomy and your doctor may remove all or part of your oesophagus. This can prevent cancer formation.
Prevention
The best way to prevent this disease is to address the symptoms of GERD and conditions like heartburn. People with frequent untreated heartburn, are more likely to develop Barret’s oesophagus or oesophageal dysplasia. You can simply follow a healthy lifestyle and avoid some triggers including:
- Eat healthy, whole, and unprocessed food
- Avoid eating large meals and take frequent short meals over the course of the day
- Avoid smoked food
- Take a walk after eating food especially after dinner
- Consult your doctor if you are experiencing persistent heartburns
- American College of Gastroenterology. Accessed 5/28/2020.Barrett’s Esophagus.(https://gi.org/topics/barretts-esophagus/)
- American Society for Gastrointestinal Endoscopy. . Accessed 5/28/2020.Understanding Barrett’s Esophagus (https://www.asge.org/home/for-patients/patient-information/understanding-barrett-39-s-esophagus)
- International Foundation for Gastrointestinal Disorders. Accessed 5/29/2020.Barrett’s Esophagus. (https://www.aboutgerd.org/barretts-esophagus.html)
- International Foundation for Gastrointestinal Disorders. . Accessed 5/28/2020.Overview: Symptoms of GERD (https://www.aboutgerd.org/signs-and-symptoms-overview.html)
- The National Institute of Diabetes and Digestive and Kidney Diseases. . Accessed 5/28/2020.Barrett’s Esophagus (https://www.niddk.nih.gov/health-information/digestive-diseases/barretts-esophagus)
- https://my.clevelandclinic.org/health/diseases/14432-barretts-esophagus
- Barrett’s esophagus. National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/digestive-diseases/barretts-esophagus/all-content. Accessed April 3, 2020.
- Iyer PG, et al. Mayo Clinic Proceedings. 2019;doi:10.1016/j.mayocp.2019.01.032.
The content shared in the Health Literacy Hub website is provided for informational purposes only and it is not intended to replace advice, diagnosis, or treatment offered by qualified medical professionals in your State or Country. Readers are encouraged to confirm the information provided with other sources, and to seek the advice of a qualified medical practitioner with any question they may have regarding their health. The Health Literacy Hub is not liable for any direct or indirect consequence arising from the application of the material provided.